Neck Pain & The Ageing Process
Posted by Phil Heler on January 5, 2016As we get older, the effects of ageing and everyday use cause wear to the vertebra, facet joints, discs and soft tissues that make up the spine.
Typical symptoms: dull neck ache and stiffness, headaches, sometimes causing radiating pain into arms and shoulders, numbness and tingling arms and hands.
As we get older, the effects of ageing and everyday use cause wear to the vertebra, facet joints, discs and soft tissues that make up the spine. Unfortunately, this goes with the territory!
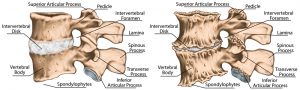
The intervertebral discs of the spine desiccate and shrink, and the ligaments and muscle tendons stiffen. Cervical spondylosis is the collective term we use for all these processes.
The discs at the bottom of your neck at C4/C5 or C5/C6 or C6/C7 are the levels most likely to suffer from cervical spondylosis as they help support most of the weight of your head. At these levels the vertebral discs are most prone to degeneration (degenerative disc disease) along with the spinal joints (facet joints) and vertebra. These gradual changes will collectively stiffen your neck and reduce your movement and, in extreme, even impinge on spinal nerves causing trapped nerves.
Our new IDD Therapy programme is effective in treating trapped nerves, is non-invasive (unlike surgery) and is pain free. IDD Therapy bridges the gap between what manual therapy cannot achieve and surgery. This therapy is the fastest growing therapy for trapped nerves and degenerative disc issues in the UK.
Bulging and herniated discs in the neck
A disc bulge is where the outer wall of the disc bulges out from its normal position. The disc wall is not broken, and the nucleus material is still contained inside the disc. As the disc bulges, it may press against nerves directly. Often bulges are associated with a loss of disc height (this happens as part of disc degeneration) and this may lead to impingement of a nerve as it exits the spinal canal though the gap between two vertebrae called a foramen.
A herniated disc is the same as a prolapsed disc. This is where the nucleus of the disc breaks through the outer disc wall. There will be a loss of disc height as the disc loses pressure and the nucleus material can press directly on to the spinal nerves causing pain. Or the material of the disc nucleus may act as a biochemical irritation to the nerve, in which case the result is the same… pain!
A ‘slipped disc’ is an everyday expression which doesn’t have a true medical definition. It can imply a disc bulge or a herniation, usually a herniation.
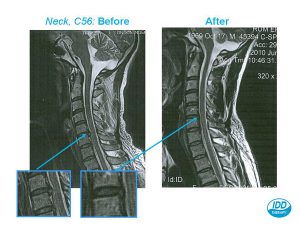
The MRI below demonstrates a disc bulge pressing on nerves in the neck. We took an MRI scan of the same patient before and after IDD Therapy (we offer this at the Buxton Osteopathy Clinic). If you look carefully you can see the disc bulge has significantly diminished allowing this person’s symptoms to fully resolve.
The resulting pain from a herniated disc will often refer (hence the term radicular pain) down the pathway of a nerve and into the limb it innervates causing either sciatica (in the case of the lower back) or pain into the neck, shoulder and arm (if in the neck). This can often be accompanied with pins and needles in the foot or hand depending on this location.
Disc issues usually occur in the same areas of the spine time after time because no matter who we are we are made the same way.
These complaints usually take time to resolve and can be very debilitating. Often the options to treat these conditions may be limited. Pain killers and manual therapy sometimes offer only limited relief. Many people may wish to avoid surgery because of its related risks. By contrast IDD is safe, non-invasive and effective. Research shows for instance that patients with a herniated disc in the lumbar spine and accompanying sciatica showed a good to excellent improvement with this mode of treatment in 86% of cases.
Our IDD Therapy programme can help treat trapped nerves, is non-invasive (unlike surgery) and is pain free. IDD Therapy bridges the gap between what manual therapy cannot achieve and surgery. This therapy is the fastest growing therapy for trapped nerves and degenerative disc issues in the UK.
Spinal stenosis in the neck
Spinal stenosis refers to a build-up of bony deposits in the vertebrae. It is typically associated with the ageing process. As we get older, in the same way that our skin ages, so too do our discs. Everyone will have degenerative discs to some degree, it goes with the territory unfortunately.
In some cases, the loss of disc height as we lose water leads to more load pressure being exerted on the vertebrae.
The body reacts to the increased load by laying down more bone to reinforce the vertebrae. In some cases, the extra bone can narrow and exert pressure on the spinal cord (central stenosis) or exiting nerve roots (lateral stenosis).
As the spinal cord is made up of nerve fibres carrying messages to the brain from the rest of the body, pressure on these nerves in the neck can produce symptoms in several parts of the body. At the more extreme end symptoms may include:
- Difficulties with walking
- Legs may feel stiff and clumsy
- Changes to the sensation in your hands (for example, it may be difficult to feel and recognise objects)
- Problems with your bladder (for example, emptying your bladder or incontinence).
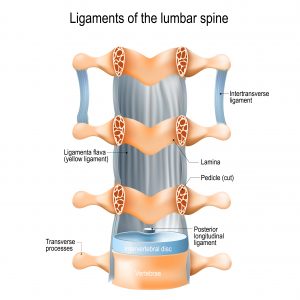
Another cause of spinal stenosis is the ligamentum flavum hypertrophy (flavum means yellow and this is really is the colour of this specific ligament).
This ligament, however, can become inflamed (hypertrophy) due to stress on the spine and this often occurs in people over the age of 50 due to the natural degeneration process of the spine.
As the structures in the spine degenerate stress increases on the ligamentum flavum. When this happens, cells in the ligament become inflamed (hypertrophy) and begin to ossify or thicken. This increase in size and decrease in elasticity occasionally combine to reduce the area available for nerve roots and the spinal cord to pass (spinal stenosis).
This degeneration can happen at any level of the spine but is most commonly experienced in the lumbar (lower back) and cervical (neck) regions.
Facet joint arthropathy in the neck
In the spine, facet joints link the vertebrae and are important for preventing excessive rotational and twisting forces which would damage the discs. They also share some of the load-bearing of the spine.
When there is a loss of mobility in the spine, the facet joints bear a greater load than normal. This is particularly the case if there is some imbalance in the body and one side of the spine takes more strain than the other.
Imbalance in weight distribution not only adds to the stress borne by the facets but effectively deteriorates bone and cartilage. Constant movement on these worn structures activates an inflammatory reaction to the joint which is full of nerve endings. The result is chronic pain as the body continuously sends pain signals to the brain.
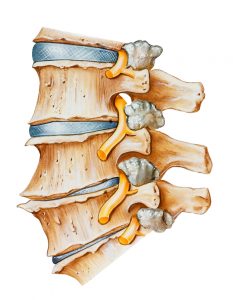
Just like the vertebra the body reacts to the increased load on the facet joints by laying down more bone in the joint margins (this is called facet joint arthropathy). In some cases, the extra bone can narrow the gap where the nerves exit the spine and if the bone pinches against the bone, it can cause referred pain into the arm.
Disc degeneration in the neck
Disc degeneration is common in the neck (cervical spine) and lower back (lumbar spine). This is because these areas of the spine undergo the most movement and stress, and are subsequently most susceptible to disc degeneration (as these bear much of our weight).
Degenerative disc disease refers to symptoms of neck pain (this can refer to the shoulder) caused by wear-and-tear on a spinal disc. In some cases, degenerative disc disease also causes weakness, numbness, and hot, shooting pains in the arms and shoulder (radicular pain). Degenerative disc disease typically consists of a low-level chronic pain with intermittent episodes of more severe pain.
The discs are made of an inner toothpaste-like substance which is mainly comprised of water that acts as a compressible fluid ball-bearing (nucleus pulposus) and an outer fibrous wall (annulus fibrosus) made of collagen.
The spongy intervertebral discs absorb shocks and pressure from the load of our bodies and squash as we lean or bend in any direction. They stop the vertebrae rubbing against each other (bone on bone) and they create a space between the vertebrae. This space is very important.
Each vertebra has a hole in the middle and when the vertebrae are stacked on top of one another combine to form a tunnel or canal through which the spinal cord travels down from the brain.
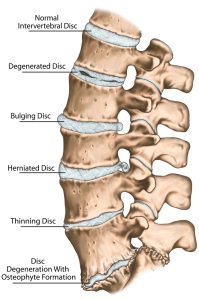
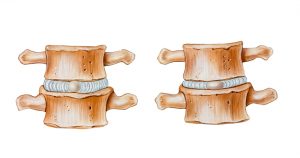
In children, the discs are about 85% water. The discs begin to naturally lose hydration during the ageing process. Some estimates have the disc’s water content typically falling to 70% by the age of 70, but in some people the disc can lose hydration much more quickly (as seen in the bottom two discs below)
As the disc loses hydration, it offers less cushioning and becomes more prone to cracks and tears. The disc is not able to truly repair itself because it does not have a direct blood supply. As such, a tear in the disc either will not heal or will develop weaker scar tissue that has potential to break again. At the same time as the disc loses moisture and its structural integrity content it will protrude and bulge and can press on nearby nerves.
Trapped nerves in the neck
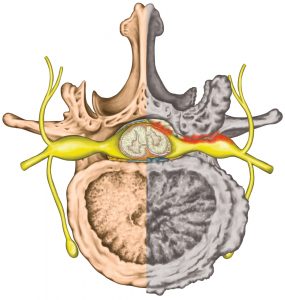
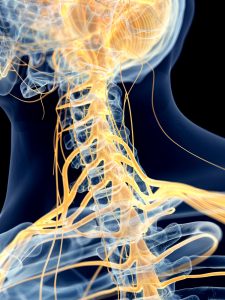
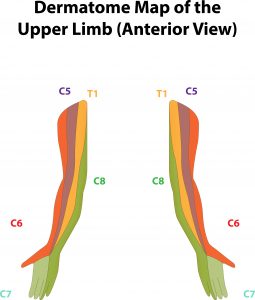
The diagram below shows the nerves in the neck and just how complex they are. Any pressure on any of these will most likely cause shoulder and arm pain with possible pins and needles into the elbow, forearm or hand with varying intensity depending on the cause.
Any of these nerves can become trapped for several different reasons and refer to the arm and shoulder.
The areas a single nerve innervates in the arm and shoulder is called a dermatome and each specific nerve will be responsible for sensory perception in different areas (temperature, touch, vibration, pressure and pain). Therefore, if a nerve is impinged in the neck, pain and pins and needles (or paraesthesia) will refer to any given dermatome.
Our IDD Therapy programme can help treat trapped nerves, is non-invasive (unlike surgery) and is pain-free. IDD Therapy bridges the gap between what manual therapy cannot achieve and surgery. This therapy is the fastest growing therapy for trapped nerves and degenerative disc issues in the UK.