The Ageing Process and Back Pain
Posted by Phil Heler on January 18, 2016The lower back (or lumbar spine) enables most of our daily duties and is therefore the focus of trauma too. Unfortunately these demands understandably impose considerable demands on the lower back and all its accompanying structures.
Your upper body is approximately two thirds of your body weight and as you lean forwards simple physics dictates that large forces will be generated. Because of these effects accumulated over time the lower back is a common focal point for wear and tear (more often referred to as lumbar spondylosis).
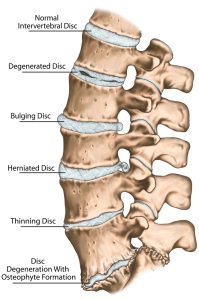
As we grow older, the effects of ageing and everyday use cause wear to the vertebra, facet joints, discs and soft tissues that make up the spine. So, what are the most common effects?
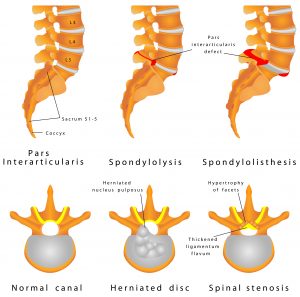
Spinal stenosis
Spinal stenosis refers to a build-up of bony deposits in the vertebrae. It is typically associated with the ageing process. As we get older, in the same way that our skin ages, so too do our discs. Everyone will have degenerative discs to some degree; it goes with the territory unfortunately.
In some cases, the loss of disc height as we lose water leads to more load pressure being exerted on the vertebrae.
The body reacts to the increased load by laying down more bone to reinforce the vertebrae. In some cases, the extra bone can narrow and exert pressure on the spinal cord (central stenosis) or exiting nerve roots (lateral stenosis).
Central stenosis as it developed will often lead to difficulties walking and your legs can feel stiff and clumsy. You may also get altered sensation in your feet and experience altered sensations in your bladder (such as issues emptying your bladder).
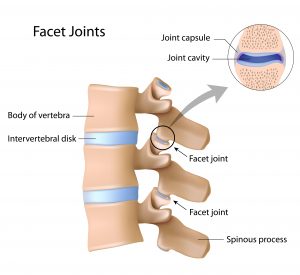
Facet joint arthropathy and spondylolisthesis
In the spine, facet joints link the vertebrae and are important for preventing excessive rotational and twisting forces which would damage the discs. They also share some of the load bearing of the spine.
When there is a loss of mobility in the spine, the facet joints bear a greater load than normal. This is particularly the case if there is some imbalance in the body and one side of the spine takes more strain than the other.
Imbalance in weight distribution not only adds to the stress borne by the facets but effectively deteriorates bone and cartilage. Constant movement on these worn structures activates an inflammatory reaction in the joint which is full of nerve endings. The result is chronic pain as the body continuously sends pain signals to the brain.
Just like the vertebra the body reacts to the increased load on the facet joints by laying down more bone in the joint margins (this is called facet joint arthropathy). This process is accentuated by degeneration of the intervertebral disc which shrink as we age, thus imposing greater load on the spinal joints.
In some cases, the extra bone can narrow the gap where the nerves exit the spine and if the bone pinches against the bone (referred to as lateral stenosis as seen under spinal stenosis), it can cause referred pain into the leg.
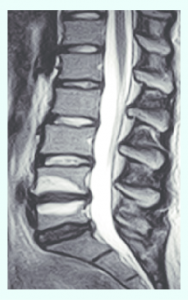
The picture below demonstrates another example of a hypertrophied facet joint.
One of the outcomes of degeneration of the facet joints and the discs can sometimes be a degenerative spondylolisthesis and this usually occurs at L3/L4 or L4/L5.
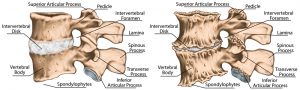
The word spondylolisthesis comes from a Latin root and means ‘slipped vertebral body’. This occurs because of a fracture in a part of the vertebra known as the ‘pars interarticularis’. This is more common if you are over 50 years of age and more common in females than males (3:1).
The term spondylolysis refers to a non-displaced fracture of the pars interarticularis as seen in the diagram. However, if the spondylolysis becomes unstable and slips forward it is termed as a spondylolisthesis.
Disc degeneration is common in the neck (cervical spine) and lower back (lumbar spine). This is because these areas of the spine undergo the most movement and stress and are subsequently most susceptible to disc degeneration (as these bear much of our weight).
Degenerative disc disease refers to symptoms caused by wear-and-tear on a spinal disc. In some cases, degenerative disc disease also causes weakness, numbness, and hot, shooting pains into the hip, groin and upper thigh (radicular pain) in the lower back. Degenerative disc disease typically consists of a low-level chronic pain with intermittent episodes of more severe pain.
The discs are made of an inner toothpaste-like substance which is mainly comprised of water (nucleus pulposus) and an outer fibrous wall (anulus fibrosus) made of collagen.
The spongy intervertebral discs absorb shocks and pressure from the load of our bodies and squash as we lean or bend in any direction. They stop the vertebrae rubbing against each other (bone on bone) and they create a space between the vertebrae. This space is very important.
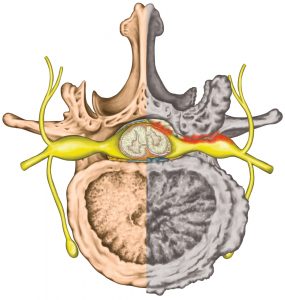
Each vertebra has a hole in the middle and when the vertebrae are stacked on top of one another combine to form a tunnel or canal through which the spinal cord travels down from the brain.
In children, the discs are about 85% water. The discs begin to naturally lose hydration during the ageing process. Some estimates have the disc’s water content typically falling to 70% by the age of 70, but in some people the disc can lose hydration much more quickly.
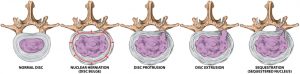
As the disc loses hydration, it offers less cushioning and becomes more prone to cracks and tears. The disc is not able to truly repair itself because it does not have a direct blood supply. As such, a tear in the disc either will not heal or will develop weaker scar tissue that has potential to break again. At the same time, as the disc loses moisture and its structural integrity content it will protrude and bulge and can press on nearly nerves.
Disc tears and annular tears
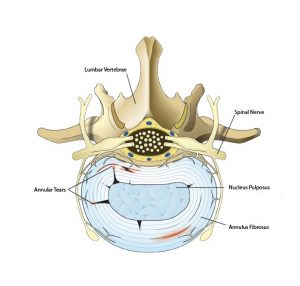
Annular tears are tears that occur inside the disc. Your discs are made of an inner toothpaste-like substance in the middle which is mainly comprised of water (nucleus pulposus) and an outer fibrous wall (anulus fibrosus) made of collagen. Annular tears are tears to the round rings of cartilage that make up the annulus fibrosis.
There are three main types of annular tears that occur in the human disc.
There is a rim lesion which is a horizontal tearing of the outer annular fibers of the disc near the outside of the disc. Typically, this type of annular tear is horizontal in nature. While the natural degeneration of the intervertebral disc is often the cause of annular tears, rim lesions are usually said to occur due to physical trauma. Discs that have the presence of rim lesions generally degenerate faster than healthy discs.
Another type of tear is a concentric term which is a splitting apart of the lamellae of the annulus in a circumferential direction. This one tends to occur in either the back (or posterior) or posterolateral region of the disc which unfortunately is where all the pain sensor are present (or nociceptors).
The radial tear, (or full thickness annular tear) is a horizontally orientated annular tear that that begins in the nucleus pulposus and then tears its way toward the periphery of the disc.
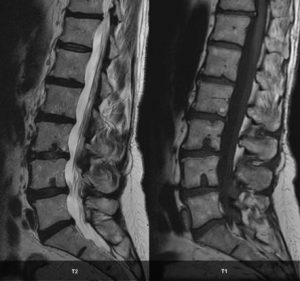
Pain from annular tears can result in pain in the lower back area, which can also extend into the buttocks, legs and sometimes down into the feet as well. The degree of pain differs from person to person and will depend the extent of the annular tears. Tingling and numbness in the lower limb can also occur. The type and severity of the tears can be diagnosed by MRI.
Deterioration of the vertebral endplate: Schmorl’s nodes and Modic changes
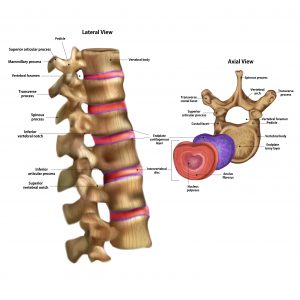
The vertebral endplate describes a thick layer of cartilage that is 0.6-1mm thick that strongly attaches to the vertebral body as seen below on the right in the axial view. These plates are interfaces between the vertebral bodies and they also have important roles in biomechanical integrity and disc nutrition.
However, the vertebral endplate also appears to be the structure of the disc that is most susceptible to mechanical failure. So what happens to it?
One common condition that occurs with ageing (although in can happen in younger people as well) is the formation of Schmorl’s nodes. This describes the process when disc material pushes through the vertebral endplate. The protrusions may contact the marrow of the vertebra, leading to inflammation.
It is believed that Schmorl nodes develop following back trauma, although this is incompletely understood. A more recent study suggests the disc puts pressure on the weakest part of the end plate.
Quiescent Schmorl nodes are extremely common found in around 75% of autopsies, at all ages, more frequently in males. They are usually asymptomatic, and their etiological significance for back pain is controversial.
Acute Schmorl nodes, in contrast, are uncommon and are associated with inflammation and symptoms. These can be seen in the MRI below where they are obvious visible protrusions into the vertebra.
Another term applied to the vertebral endplate are Modic changes. This is a term which is used to describe the changes of the vertebral endplate that are related to spinal degeneration. These were first described by Dr. Modic, who was the first doctor to identify and classify degenerative endplate changes and marrow changes in the vertebra surrounding the intervertebral disc.
These changes can be seen by MRI and have been classified from Types 1-3. These changes generally happen in the lower back most commonly at L4/L5 and L5/S1. Once changes occur they generally progress from Type 1 to Type 2 (and to Type 3). Type 1 changes can be seen in the MRI below at the L4 and L5 as displayed by the lighter areas.
Type 2 represents replacement of bone in the vertebra with fatty tissue marrow. Type 3 describes replacement of bone with bony sclerosis and the vertebra loose trabeculation (this is what gives bone structural support).
75 –80 % of patients who have Modic changes have constant pain, without a pain-free moment day or night. It is difficult to treat and normal treatment that normally cures or help patients with normal back pain does not have an effect on Modic changes or pain from Modic changes.